FAQ
- What is a Pediatric Dentist?
- Your Child's First Dental Visit
- Why are the Primary Teeth so Important?
- Dental X-rays
- ToothPrints I.D.
- Dental Treatment for Children with Special Needs
- Care of Your Child's Teeth
- Good Diet = Healthy Teeth
- How do I Prevent Cavities?
- Seal Out Decay
- Baby Bottle Tooth Decay (Early Childhood Caries)
- When Will my Baby Start Getting Teeth?
- Eruption of Your Child's Teeth
- Dental Emergencies
- Fluoride
- Fluoride Awareness Survey
- What's the Best Toothpaste for my Child?
- Fillings
- Nitrous Oxide
- Does Your Child Grind his Teeth at Night? (Bruxism)
- Thumb Sucking
- Tongue Piercing - Is it Really Cool?
- Tobacco - Bad News in Any Form
- What is the Best Time for Orthodontic Treatment?
- Mouth Guards
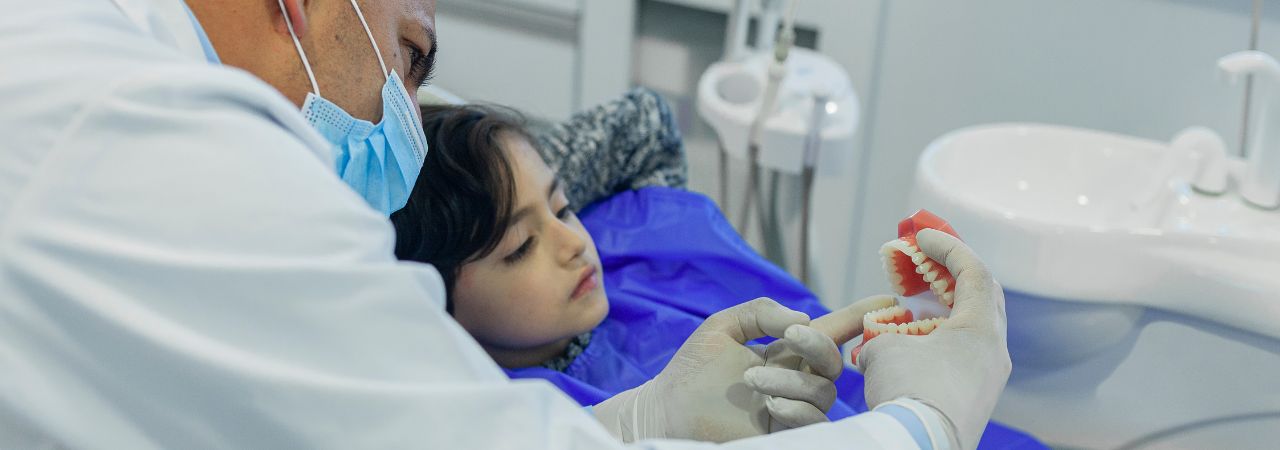
What is a Pediatric Dentist?
 The pediatric dentist has an extra two years of specialized training and is dedicated to the oral health of children from infancy through the teenage years. The very young, pre-teens and teenagers all need different approaches in dealing with their behavior, guiding their dental growth and development, and helping them avoid future dental problems. The pediatric dentist is best qualified to meet these needs.
The pediatric dentist has an extra two years of specialized training and is dedicated to the oral health of children from infancy through the teenage years. The very young, pre-teens and teenagers all need different approaches in dealing with their behavior, guiding their dental growth and development, and helping them avoid future dental problems. The pediatric dentist is best qualified to meet these needs.
Your Child's First Dental Visit
According to the American Academy of Pediatric Dentistry (AAPD), your child should visit the dentist by his/her 1st birthday. You can make the first visit to the dentist enjoyable and positive. Your child should be informed of the visit and told that the dentist and his staff will explain all procedures and answer any questions. The less to-do concerning the visit, the better.
It is best if you refrain from using words around your child that might cause unnecessary fear, such as needle, pull, drill or hurt. Pediatric dental offices make a practice of using words that convey the same message, but are pleasant and non-frightening to the child.
Why are the Primary Teeth so Important?
It is very important to maintain the health of the primary teeth. Neglected cavities can and frequently do lead to problems which affect developing permanent teeth. Primary teeth, or baby teeth, are important for (1) proper chewing and eating, (2) providing space for the permanent teeth and guiding them into the correct position, and (3) permitting normal development of the jaw bones and muscles. Primary teeth also affect the development of speech and add to an attractive appearance. While the front 4 teeth last until 6-7 years of age, the back teeth (cuspids and molars) aren't replaced until age 10-13.
Dental X-rays
Radiographs (X-rays) are a vital and necessary part of your child's dental diagnostic process. Without them, certain dental conditions can and will be missed.
X-ray's detect much more than cavities. For example, X-rays may be needed to survey erupting teeth, diagnose bone diseases, evaluate the results of an injury, or plan orthodontic treatment. X-rays allow dentists to diagnose and treat health conditions that cannot be detected during a clinical examination. If dental problems are found and treated early, dental care is more comfortable for your child and more affordable for you.
The American Academy of Pediatric Dentistry recommends X-rays and examinations every six months for children with a high risk of tooth decay. On average, most pediatric dentists request radiographs approximately once a year. Approximately every three years it is a good idea to obtain a complete set of radiographs, either a panoramic and bitewings or periapicals and bitewings.
Pediatric dentists are particularly careful to minimize the exposure of their patients to radiation. With contemporary safeguards, the amount of radiation received in a dental X-ray examination is extremely small. The risk is negligible. In fact, the dental X-rays represent a far smaller risk than an undetected and untreated dental problem. Lead body aprons and shields will protect your child. Today's equipment filters out unnecessary X-rays and restricts the X-ray beam to the area of interest. High-speed film and proper shielding assure that your child receives a minimal amount of radiation exposure.
Toothprints® I.D.
Click here to view the Curriculum Vitae of David A. Tesini (Developer of Toothprints)
 The Dental I.D. for Safeguarding Children
The Dental I.D. for Safeguarding Children
One of the greatest fears of parents today are that their children will be lost or stolen. Toothprints® is a simple technique for documenting tooth and jaw characteristics and provides parents with additional piece of mind.  This program was developed by Dr. David Tesini and is offered to all our patients free of charge. The toothprint program is highly acclaimed nation-wide and has been incorporated into the Massachusetts Child Identification Program(CHIP).
This program was developed by Dr. David Tesini and is offered to all our patients free of charge. The toothprint program is highly acclaimed nation-wide and has been incorporated into the Massachusetts Child Identification Program(CHIP).
Toothprints® is an arch-shaped thermoplastic wafer that you soften in hot water, then placed on the patient's lower arch. The child bites into the wafer for 50 seconds and then a 2-3 cool down period allows the toothprint to be placed in a bag and sent home with the parents for safe keeping.
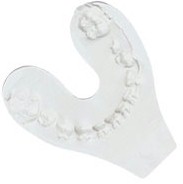 Toothprints® should be done at least every 2-3 years with minimum requires been;
Toothprints® should be done at least every 2-3 years with minimum requires been;
- initial impression: Age 3 (or after all primary teeth have erupted)
- Update: Age 7 or 8 (or after the upper and lower incisors and the first permanent molars have erupted)
- Update: Age 12 or 13 (or after all permanent, excluding 3rd molars, have erupted)
Remember, the TOOTHPRINTS I.D. PROGRAM is free to our patients. Call us for more information and schedule an appointment that will only take a few minutes.
MYCHIP.ORG - Parents can find community and educational programs in Massachusetts by clicking on mychip.org. The dentist can make them for your child.
Your child's safety is important to us! No one has a bite like yours.
Dental Treatment for Children with Special Needs
For information on special oral health care needs, we've provided links to the following sites:
The American Dental Association
Just For Kids
Word of Mouth
American Academy of Pediatric Dentistry
Dental Related Internet Resources
Project Stretch
Healthy People 2001
Sports Dentistry on Line
National Institute of Dental & Craniofacial Research
Resource & Information on Cleft Lip & Palate
National Foundation for Ectodermal Dysplasias
FINDING YOUR CAR IN THE PARKING LOT;
The Role of Parents and Direct Support Professionals in Providing Attention
to Oral Healthcare Needs of the Child with Special Needs.
A vast amount of information is available and awaits us at every turn, in all media forms, and through every contact with our healthcare providers. Pamphlets, articles, booklets, the internet, newsletters, magazines... all provide access to oral health knowledge that we all need to have. We read about brushing and flossing, the importance of periodic dental visits, diet and nutrition, protection of teeth at Special Olympic events and during other sports, early treatment of crooked teeth, the importance of fluoride, and the list goes on. We have seen pictures severe gum disease, malocclusions and broken teeth, while Web sites direct us to dental offices which provide services to our children. Articles tell stories of unmet dental needs in the special patient population, and about how to deal with the financial restraints put on both patients and providers.
Don't be nervous or afraid to bring your very young child to the dentist because you think that either the dentist will be hard to deal with or it may be difficult for the dentist to deal with your child, and therefore worried the experience will be a disaster. The longer you wait, the harder it may be.
If only we could pull in to a parking lot, get out of the car, head toward the neon sign that reads "Same-day Dental Care Here", and stroll back to the car and exit with perfect pearly whites. The typical dental journey, however, sends us in so many directions that when we come out we cannot even find our car in the parking lot. What can we do?
Plain and simple, good oral hygiene begins at home and it begins early-- soon after the primary tooth erupts. Good oral health requires discipline and parents and caregivers need only follow these four simple steps to assure a healthy smile:
Step 1: Early infant oral care is important for all children.
Step 2: Start looking for a dentist NOW.
Step 3: Do your part: Keep your appointments.
Step 4: Advocate as part of the team.
Children with special needs need a head start.
Many children with special needs develop jaw growth and tooth alignment problems early. Although recognized by dentists, parents and DSP's many times these malocclusions are left untreated simply because the child has a disability. We need to remember, the only reason for not doing orthodontic treatment is poor oral hygiene or unmanageable behavior, both of which have potential for improvement. The presence of a disability is NOT a contraindication to receiving orthodontic treatment. Parents need to work with their child's dentist to be sure that specialized therapy, such as periodontia or orthodontia, is improved. Start early... be disciplined... be part of the dental team; the reward will be in your child's smile for a lifetime and you will always be able to find your car in the parking lot.
Dr. David Tesini
Past President of the Academy of Dentistry for persons with disabilities.
Care of Your Child's Teeth
 Begin daily brushing as soon as the child's first tooth erupts. A pea-size amount of fluoride toothpaste can be used after the child is old enough not to swallow it. By age 4 or 5, children should be able to brush their own teeth twice a day with supervision until about age seven to make sure they are doing a thorough job. However, each child is different. Your dentist can help you determine whether the child has the skill level to brush properly.
Begin daily brushing as soon as the child's first tooth erupts. A pea-size amount of fluoride toothpaste can be used after the child is old enough not to swallow it. By age 4 or 5, children should be able to brush their own teeth twice a day with supervision until about age seven to make sure they are doing a thorough job. However, each child is different. Your dentist can help you determine whether the child has the skill level to brush properly.
Proper brushing removes plaque from the inner, outer and chewing surfaces. When teaching children to brush, place toothbrush at a 45 degree angle; start along gum line with a soft bristle brush in a gentle circular motion. Brush the outer surfaces of each tooth, upper and lower. Repeat the same method on the inside surfaces and chewing surfaces of all the teeth. Finish by brushing the tongue to help freshen breath and remove bacteria.
Flossing removes plaque between the teeth where a toothbrush can't reach. Flossing should begin when any two teeth touch. You should floss the child's teeth until he or she can do it alone. Use about 18 inches of floss, winding most of it around the middle fingers of both hands. Hold the floss lightly between the thumbs and forefingers. Use a gentle, back-and-forth motion to guide the floss between the teeth. Curve the floss into a C-shape and slide it into the space between the gum and tooth until you feel resistance. Gently scrape the floss against the side of the tooth. Repeat this procedure on each tooth. Don't forget the backs of the last four teeth.
Good Diet = Healthy Teeth
Healthy eating habits lead to healthy teeth. Like the rest of the body, the teeth, bones and the soft tissues of the mouth need a well-balanced diet. Children should eat a variety of foods from the five major food groups. Most snacks that children eat can lead to cavity formation. The more frequently a child snacks and the types of snacks they eat can lead to a greater chance of tooth decay. How sticky a snack is and how long they stay in your mouth play a important role. Sticky snacks, especially if they are high in sugar, i.e., fruit roll-ups, stick to the biting surfaces of the teeth and removal is very difficult. How long food remains in your mouth also plays a role. Breath mints and hard candy stay in the mouth a long time, which causes longer acid attacks on tooth enamel. If your child must snack, choose nutritious foods such as vegetables, low-fat yogurt, and low-fat cheese which are healthier and better for your child's teeth.
How do I Prevent Cavities?
Good oral hygiene removes bacteria and the leftover food particles that combine to create cavities. For infants, use a wet gauze or clean washcloth to wipe the plaque from teeth and gums. Avoid putting your child to bed with a bottle filled with anything other than water.
For older children, brush their teeth at least twice a day. Also, watch the number of snacks containing sugar that you give your children.
The American Academy of Pediatric Dentistry recommends six month visits to the pediatric dentist beginning at your child's first birthday. Routine visits will start your child on a lifetime of good dental health.
Your pediatric dentist may also recommend protective sealants or home fluoride treatments for your child. Sealants can be applied to your child's molars to prevent decay on hard to clean surfaces.
 | Look Mom...No Cavities! / How To Raise A Cavity-Free Child |
Seal Out Decay
A sealant is a clear or shaded plastic material that is applied to the chewing surfaces (grooves) of the back teeth (premolars and molars), where four out of five cavities in children are found. This sealant acts as a barrier to food, plaque and acid, thus protecting the decay-prone areas of the teeth.
Baby Bottle Tooth Decay (Early Childhood Caries)
One serious form of decay among young children is baby bottle tooth decay. This condition is caused by frequent and long exposures of an infant's teeth to liquids that contain sugar. Among these liquids are milk (including breast milk), formula, fruit juice and other sweetened drinks.
Putting a baby to bed for a nap or at night with a bottle other than water can cause serious and rapid tooth decay. Sweet liquid pools around the child's teeth giving plaque bacteria an opportunity to produce acids that attack tooth enamel. If you must give the baby a bottle as a comforter at bedtime, it should contain only water. If your child won't fall asleep without the bottle and its usual beverage, gradually dilute the bottle's contents with water over a period of two to three weeks.
After each feeding, wipe the baby's gums and teeth with a damp washcloth or gauze pad to remove plaque. The easiest way to do this is to sit down, place the child's head in your lap or lay the child on a dressing table or the floor. Whatever position you use, be sure you can see into the child's mouth easily.
When Will my Baby Start Getting Teeth?
Teething, the process of baby (primary) teeth coming through the gums into the mouth, is variable among individual babies. Some babies get their teeth early and some get them late. In general the first baby teeth are usually the lower front (anterior) teeth and usually begin erupting between the age of 6-8 months.
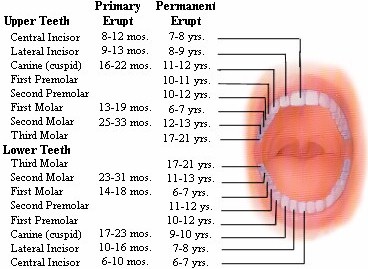
Eruption of Your Child's Teeth
Children's teeth begin forming before birth. As early as 4 months, the first primary (or baby) teeth to erupt through the gums are the lower central incisors, followed closely by the upper central incisors. Although all 20 primary teeth usually appear by age 3, the pace and order of their eruption varies.
Permanent teeth begin appearing around age 6, starting with the first molars and lower central incisors. This process continues until approximately age 21.
Adults have 28 permanent teeth, or up to 32 including the third molars (or wisdom teeth).
TOOTH DEVELOPMENT
 | Look! My Tooth is Loose! By: Patricia Brennan Demuth |
Dental Emergencies
Toothache: Clean the area of the affected tooth thoroughly. Rinse the mouth vigorously with warm water or use dental floss to dislodge impacted food or debris. DO NOT place aspirin on the gum or on the aching tooth. If face is swollen apply cold compresses. Take the child to a dentist.
Cut or Bitten Tongue, Lip or Cheek: Apply ice to bruised areas. If there is bleeding apply firm but gentle pressure with a gauze or cloth. If bleeding does not stop after 15 minutes or it cannot be controlled by simple pressure, take child to hospital emergency room.
Knocked Out Permanent Tooth: Find the tooth. Handle the tooth by the crown, not the root portion. You may rinse the tooth but DO NOT clean or handle the tooth unnecessarily. Inspect the tooth for fractures. If it is sound, try to reinsert it in the socket. Have the patient hold the tooth in place by biting on gauze. If you cannot reinsert the tooth, transport the tooth in a cup containing the patient's saliva or milk. The tooth may also be carried in the patient's mouth. The patient must see a dentist IMMEDIATELY! Time is a critical factor in saving the tooth.
Fluoride
The use of fluoride has been found to be a major factor in the reduction of dental caries. When use appropriately fluoride is both safe and effective. Fluoride is found in many different sources and frequent exposure to small amounts each day will best reduce the risk of dental caries. Drinking fluoridated water and using a toothpaste containing fluoride to brush with at least twice a day goes a long way in preventing dental decay. If you are uncertain whether you are in a fluoridated water community, call your local water utilities to be sure.
Other sources of fluoride such as fluoride drops, tablets, and rinses should only be used on the advice of your dentist, to insure that you are not getting too little or too much fluoride. Too little fluoride will not strengthen the teeth enough to prevent cavities and too much fluoride can cause fluorosis, which is a chalky to even a brown discoloration of the permanent teeth. Using a fluoride toothpaste and a topical application every six month on your recall appointment in conjunction with fluoridated water supply is all most patients require to achieve an appropriate fluoride intake. However for those patients that present with a high caries rate your pediatric dentist my recommend toothpaste that contain higher levels of fluoride and rinses to help reduce the number of caries.
Fluoride Source Awareness
Please print and complete the Fluoride Source Awareness Survey. This survey is intended to increase parents' awareness of the potential sources of fluoride which your child is receiving from a variety of sources.
To print the survey you will need Adobe Acrobat Reader. If you do not have Adobe Acrobat, please click here to download it for free to your computer.
Click here to print the Fluoride Source Awareness Survey
What's the Best Toothpaste for my Child?
Tooth brushing is one of the most important tasks for good oral health. Many toothpastes, and/or tooth polishes, however, can damage young smiles. They contain harsh abrasives which can wear away young tooth enamel. When looking for a toothpaste for your child make sure to pick one that is recommended by the American Dental Association. These toothpastes have undergone testing to insure they are safe to use.
Remember, children should spit out toothpaste after brushing to avoid getting too much fluoride. If too much fluoride is ingested, a condition known as fluorosis can occur. If your child is too young or unable to spit out toothpaste, consider providing them with a fluoride free toothpaste, using no toothpaste, or using only a "smidgen" of toothpaste.
Fillings
If your child is diagnosed with a cavity, based on what the doctor has seen on an X-ray or in the mouth, the material used for your child's filling will be either resin (tooth-colored) or amalgam (silver). The amalgam filling is a mechanical bond involving removal of more tooth structure than a resin filling. While amalgam may still be recommended in the rare event of a deep cavity, a resin filling will more likely be recommended as it is a chemical bond and requires removal of less of the tooth structure. Although resin is a significantly more expensive material to use and a more expensive procedure to deliver, the charge for an amalgam and a resin filling are the same.
We no longer do silver (amalgam) fillings on primary (baby) teeth due to the substantial improvement in composite filling materials. These new materials have been found to perform better than the amalgam restorations on primary teeth. We may still recommend, on occasion, silver (amalgam) fillings in certain cases for permanent molars. Please be aware that your insurance company may not pay for a resin filling at the same level as amalgam or in some cases will not pay at all for resin fillings.
Resin fillings are not a covered expense for Delta Dental Plan and Blue Cross Blue Shield of Massachusetts. However, in some instances these plans will pay for the resin filling at the amalgam rate. Even in these cases, there will still be a significant co-payment due to contractual constraints imposed upon us. This co-payment is the member's responsibility. All plans are different and it is very important if finances are a concern to file a pretreatment estimate with your insurance for the treatment plan recommended. We will be happy to do that for you at your request. A phone call to your insurance may not give you an accurate answer.
In every case the dentist will make the recommendation as to the material to use that is in your child's best interest. Please discuss the treatment beforehand if you have a concern about the recommendation made. We welcome your input.
About Nitrous Oxide
"Nitrous Oxide is offered as an option to assist in treating your child. Nitrous Oxide is an inhaled anti-anxiety agent more commonly known as "laughing gas" because of its effects. It is delivered to your child via a nasal mask, which is placed over your child's nose.
During the appointment your child needs to be able to breathe through his/her nose. Nasal congestion would not allow nasal respiration, which would make the Nitrous Oxide ineffective. If nasal congestion is present, then the appointment must be rescheduled.
It is not necessary for your child to fast before his/her visit. We recommend a light meal because anxiety may make your child feel light-headed if his/her blood sugar is low. And so, it is fine to eat or drink, but not too heavily.
Any female that remains in the treatment room with your child must not be pregnant.
Nitrous Oxide does not eliminate the need for local anesthesia such as "Novocain." Any procedure that would need anesthesia without Nitrous Oxide, would also need anesthesia when Nitrous Oxide is used.
At the end of the visit, your child will be breathing 100% oxygen. The Nitrous Oxide will be totally removed from his/her system.
If local anesthesia has been administered, it will take a while to wear off. You will be given instructions on what to do following any local anesthesia.
The appointment for use of Nitrous Oxide entails office preparation and exclusive reservation of office space. Cancellation of an appointment with less than 24 hours' notice, or a missed appointment, will result in a charge of $75.
If you have any questions on this important matter, please ask one of our clinical staff. We will be happy to assist you.
Important note: Administration of Nitrous Oxide is not a covered service by any insurance company. Thank you for paying for this procedure on the date of service."
Does Your Child Grind his Teeth at Night? (Bruxism)
Parents are often concerned about the nocturnal grinding of teeth (bruxism). Often, the first indication is the noise created by the child grinding on their teeth during sleep. Or, the parent may notice wear (teeth getting shorter) to the dentition. One theory as to the cause involves a psychological component. Stress due to a new environment, divorce, changes at school; etc. can influence a child to grind their teeth. Another theory relates to pressure in the inner ear at night. If there are pressure changes (like in an airplane during take-off and landing when people are chewing gum, etc. to equalize pressure) the child will grind by moving his jaw to relieve this pressure.
The majority of cases of pediatric bruxism do not require any treatment. If excessive wear of the teeth (attrition) is present, then a mouth guard (night guard) may be indicated. The negatives to a mouth guard are the possibility of choking if the appliance becomes dislodged during sleep and it may interfere with growth of the jaws. The positive is obvious by preventing wear to the primary dentition.
The good news is most children outgrow bruxism. The grinding gets less between the ages 6-9 and children tend to stop grinding between ages 9-12. If you suspect bruxism, discuss this with your pediatrician or pediatric dentist.
Thumb Sucking
Sucking is a natural reflex and infants and young children may use thumbs, fingers, pacifiers and other objects on which to suck. It may make them feel secure and happy or provide a sense of security at difficult periods. Since thumb sucking is relaxing, it may induce sleep.
Thumb sucking that persists beyond the eruption of the permanent teeth can cause problems with the proper growth of the mouth and tooth alignment. How intensely a child sucks on fingers or thumbs will determine whether or not dental problems may result. Children who rest their thumbs passively in their mouths are less likely to have difficulty than those who vigorously suck their thumbs.
Children should cease thumb sucking by the time their permanent front teeth are ready to erupt. Usually, children stop between the ages of two and four. Peer pressure causes many school-aged children to stop.
Pacifiers are no substitute for thumb sucking. They can affect the teeth essentially the same way as sucking fingers and thumbs. However, use of the pacifier can be controlled and modified more easily than the thumb or finger habit. If your child uses a pacifier, use a clean pacifier - one recommended by your child's doctor or dentist. Never dip the pacifier into any sweet substance.
You can only intervene successfully when the child says "YES" and wants to stop. "GETTING TO YES" involves three steps:
Step One: Awareness of the habit; this step deals with making the child aware of his/her habit and then asking if he/she wants to stop.
Step Two: This step deals with showing the child that the thumb sucking habit is undesirable.
Step Three: Possible interventions to discuss with the pediatric dentist include:
- POSITIVE REINFORCEMENT
- CHARTS
- MITTENS
- BAND-AIDS
- 'THUMBS AWAY'
- ELBOW PADS
- ORAL APPLIANCES
Please talk to your dentist or hygienist if you have any questions or concerns.
 Harold's Hideaway Thumb |
 David Decides About Thumbsucking - A Story for Children, a Guide for Parents |
Tongue Piercing - Is it Really Cool?
You might not be surprised anymore to see people with pierced tongues, lips or cheeks, but you might be surprised to know just how dangerous these piercings can be.
There are many risks involved with oral piercings including chipped or cracked teeth, blood clots, or blood poisoning. Your mouth contains millions of bacteria, and infection is a common complication of oral piercing. Your tongue could swell large enough to close off your airway!
Common symptoms after piercing include pain, swelling, infection, an increased flow of saliva and injuries to gum tissue. Difficult-to-control bleeding or nerve damage can result if a blood vessel or nerve bundle is in the path of the needle.
So follow the advice of the American Dental Association and give your mouth a break - skip the mouth jewelry.
Tobacco - Bad News in Any Form
Tobacco in any form can jeopardize your child's health and cause incurable damage. Teach your child about the dangers of tobacco.
Smokeless tobacco, also called spit, chew or snuff, is often used by teens who believe that it is a safe alternative to smoking cigarettes. This is an unfortunate misconception. Studies show that spit tobacco may be more addictive than smoking cigarettes and may be more difficult to quit. Teens who use it may be interested to know that one can of snuff per day delivers as much nicotine as 60 cigarettes. In as little as three to four months, smokeless tobacco use can cause periodontal disease and produce pre-cancerous lesions called leukoplakias.
If your child is a tobacco user you should watch for the following that could be early signs of oral cancer:
- A sore that won't heal.
- White or red leathery patches on the lips, and on or under the tongue.
- Pain, tenderness or numbness anywhere in the mouth or lips.
- Difficulty chewing, swallowing, speaking or moving the jaw or tongue; or a change in the way the teeth fit together.
Because the early signs of oral cancer usually are not painful, people often ignore them. If it's not caught in the early stages, oral cancer can require extensive, sometimes disfiguring, surgery. Even worse, it can kill.
Help your child avoid tobacco in any form. By doing so, they will avoid bringing cancer-causing chemicals in direct contact with their tongue, gums and cheek.
What is the Best Time for Orthodontic Treatment?
Developing malocclusions, or bad bites, can be recognized as early as 2-3 years of age. Often, early steps can be taken to reduce the need for major orthodontic treatment at a later age.
Stage I - Early Treatment: This period of treatment encompasses ages 2 to 6 years. At this young age, we are concerned with underdeveloped dental arches, the premature loss of primary teeth, and harmful habits such as finger or thumb sucking. Treatment initiated in this stage of development is often very successful and many times, though not always, can eliminate the need for future orthodontic/orthopedic treatment.
Stage II - Mixed Dentition: This period covers the ages of 6 to 12 years, with the eruption of the permanent incisor (front) teeth and 6 year molars. Treatment concerns deal with jaw malrelationships and dental realignment problems. This is an excellent stage to start treatment, when indicated, as your child's hard and soft tissues are usually very responsive to orthodontic or orthopedic forces.
Stage III - Adolescent Dentition: This stage deals with the permanent teeth and the development of the final bite relationship.
Mouth Guards
When a child begins to participate in recreational activities and organized sports, injuries can occur. A properly fitted mouth guard, or mouth protector, is an important piece of athletic gear that can help protect your child's smile, and should be used during any activity that could result in a blow to the face or mouth.
Mouth guards help prevent broken teeth, and injuries to the lips, tongue, face or jaw. A properly fitted mouth guard will stay in place while your child is wearing it, making it easy for them to talk and breathe.
A custom mouth guard has the most superior fit and comfort level. An impression is taken in the dental office and a guard is made to fit the mold. They come in a variety of colors and are perfect for those that have completed orthodontic treatment and have all permanent teeth.
Another alternative is a customized boil-and-form mouth guard that may be purchased at a sports store or pharmacy. The guard is dipped in boiled water for 30 seconds and then placed in the mouth, the patient bites for a customized fit. Although the fit is not as good as the customized guard, it is good for those patients that have teeth coming in and out and may need more than one guard during the season. Stock mouth guards are one-size-fits-all. They have the least amount of retention and fit but are far better than wearing nothing at all.
